I wish I had kept a diary of Lennon’s Neonatal Intensive Care (NICU) days.
Looking through the many photos through that period of my life, it feels like only yesterday we were on that multi hospital rollercoaster ride, yet in another way it feels like it was the 11 years ago that it very nearly is.
I was a sad person then – devastated that my body was unable to carry my precious baby boy to term. I just about managed 28 weeks of pregnancy. Frightened that my baby wouldn’t survive the awful lifesaving support and treatments he needed to undergo just to give him that small flicker of a chance at life.
I was tired and desperately sad.
Lennon was transferred from the QE2 Hospital in Welwyn Garden City to Chelsea and Westminster when he was just 2 days old. He needed an oscillating ventilator and the nearest unit with one available was Chelsea. The night they moved Lennon I was still recovering from a caesarean section and preeclampsia, the midwives wouldn’t let me travel with Lennon and refused to discharge me. I stood by Lennon’s incubator for hours whilst the specialist transport team prepared to take Lennon on the 1 hour journey. It took them over 8 hours to stabilise him for the journey. At one point they debated whether or not it was safe enough to transfer him at all, and questioned the likelihood of him surviving the journey to Chelsea.
I lay in my hospital bed that night, on a maternity ward full of crying babies and wept. Tears upon tears for the baby I wished were in my arms, the baby I may never see alive again.
Late the next evening I discharged myself, still suffering the effects of the preeclampsia, but desperate to see my baby. I was an emotional mess. Walking out of the hospital with an empty womb and empty arms was the hardest experience of my life up until that point. We found a late night chemist, I needed a breast pump.
It wasn’t supposed to be like this – We were supposed to be walking out of the hospital with our baby, heading home full of happiness and excitement, ready to begin our journey into parenthood.
Ian’s father had travelled to Chelsea and Westminster hospital that afternoon. He waited hours for the nurses to get Lennon stable enough for a visitor. The staff informed Lennon’s grandfather that Lennon was extremely unwell and that they were deeply concerned about his critical condition. He couldn’t get much sicker.
The following day we made it to Chelsea and the plan was for Ian and I to stay there for a few nights, or at least until Lennon’s condition improved. My tiny baby boy looked so poorly. He was covered in wires, tubes, probes and monitors. He looked bigger than the other babies – At his birth weight – 2lb 9oz, Lennon was more than double the weight of most of the other babies on the unit, but was by far the sickest at that point. He needed so much support to stay alive. I now know the reasons behind the high level of support and why he needed all the IV infusions and treatments.

TPN because he couldn’t tolerate any feed into his stomach.
Medicines to bring up his dangerously low blood pressure and blood sugars.
Anti-biotics to rid the sepsis that was taking over his small body.
An oscillating ventilator for his paper thin lungs that couldn’t cope with the ‘normal’ breathing pattern of a conventional ventilator.
Medicine to try to close a large hole in his heart.
Needles into his bladder to attempt to find the reason for his kidney failure.
A light for his Jaundice (a bit like a sunbed – He even had a super cute eye mask!).
A lumbar puncture to check for meningitis
Daily blood transfusions.
The list goes on…..
I was scared. My baby looked so fragile and vulnerable. I wanted to be close to him but he hated being touched, every time anyone put a hand into the incubator he would drop his oxygen saturations and his blood pressure – it felt like he was communicating to us that he just wanted to be left alone. That he was scared we would break him.
I spent endless hours sitting by Lennon’s incubator, listening to the radio that was kept by his bedside, reading his charts and questioning everything that was recorded. Through the clear Perspex wall of the incubator I willed him to stay alive – begged him to stay alive and let me have a chance to be his mummy.
It was December and the run up to Christmas, joy and happiness were everywhere. Lights, decorations, gifts, people on the streets smiling and laughing, the underground full of tipsy workers traveling home from their Christmas celebrations. I wanted the whole world to stop – just like mine had. My sad face and heavy heart didn’t fit in. I didn’t want to be in this limbo. One evening after leaving the hospital I contemplated walking out on the Fulham Road into the path of an oncoming bus. I felt out of control and so low.
Days turned in to weeks and Lennon began to improve very, very slowly. This was the rollercoaster we had been told to expect – Two steps forward, one step back. It was 3 weeks before we held Lennon for the first time – Christmas Eve.
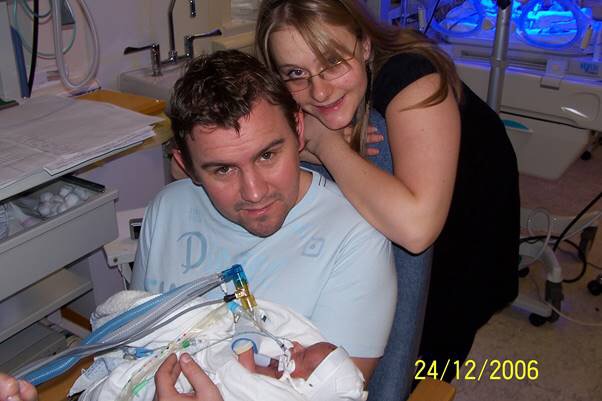

It was all I wanted for Christmas for that year, to be able to hold my baby in my arms. It wasn’t an easy task for the nurses; Lennon was still unstable and attached to so many machines and IV pumps. But they managed it and my much wanted and needed Christmas wish was granted.
6 weeks after Lennon first arrived at Chelsea and Westminster he was taken off the ventilator and was now dependant on CPAP to aid his own breathing. He still needed a fair amount of IV support, but seemed to be tolerating small feeds into a Nasal Gastric (NG) tube. And so we were transferred back to Lister Hospitals NICU in Stevenage, much closer to home. We were over the moon – One step closer to home! Shorter journeys to the hospital also meant I could spend much more time with Lennon, and the visiting hours at Lister were much less strict than they were at Chelsea.
Lennon spent the following 6 weeks dependant on CPAP. We were able to hold him most days, he had his first bath, and despite Lennon still being in an incubator because he was unable to support his own temperature, we were encouraged to get him dressed every day.
By the time Lennon had reached his due date – 27th February 2007, he was in the Special Care room and only needed nasal cannula oxygen to help with his breathing. He was prescribed an array of medication, and although he still needed his NG tube he taking a small amount of feed orally. He occasionally would stop breathing and needed to be resuscitated. It was scary, but it was nothing we hadn’t gotten used to seeing over the last couple of months. Things were looking up and home had been discussed a few times. Both Ian and I were understandably delighted by the slightest mention of bringing Lennon home, although at the same time nervous about caring for an oxygen dependant baby needing tube feeds. And the thought of him stopping breathing at home petrified me, but I really wanted my baby at home, where he belonged.
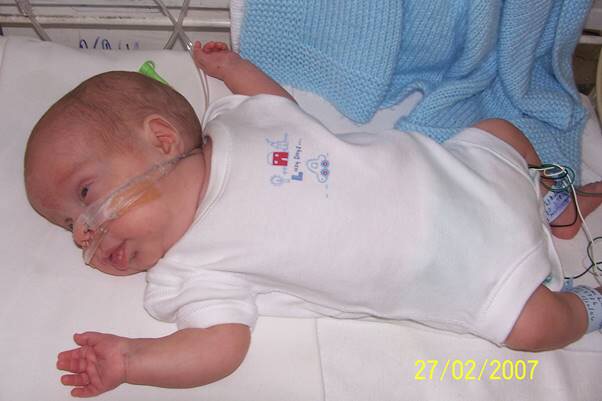
Unfortunately this wasn’t to be. Lennon had other ideas – his breathing deteriorated quite rapidly over the course of a few days, until he needed to be intubated and ventilated again. That day will stay with me forever. I relive that day many times in my head, repaying the scenario minute by minute.
The Doctor reviewing Lennon and transferring him back into the NICU room.
The look on all the nurses’ faces and the tears in their eyes.
The mum that took me out of the room to call Ian and tell him to get there as quickly as he could.
Being led to the ‘bad news’ room and sitting in silence, alone, waiting for someone to tell me my baby hadn’t made it this time.
Ian arriving, crying on my shoulder.
Being led back to Lennon and asking if the nurse if he was going die and her replying that she couldn’t answer me.
Drinking copious amounts of sugary tea…..
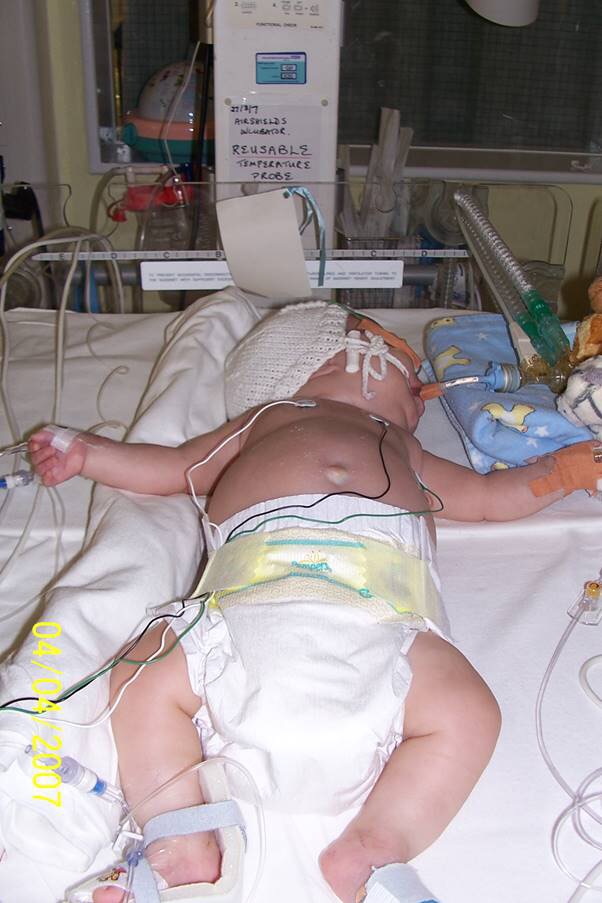
No one could find a reason why Lennon had suddenly become ventilator dependant again. All sorts of doctors visited to NICU to review him. They suspected Lennon had chronic renal failure and an endocrine issue but nothing that would hinder his ability to breathe unaided. They even called in an adult cardiac doctor who carried out extensive test – they all came back normal. I was devastated. We had tumbled so far backwards. I returned to sitting helpless at Lennon’s bed side. I read him stories and learnt to crochet to help pass the time.
Winter turned to spring and we were still in NICU at Lister holding a bedside vigil, whilst waiting for a bed to become available on the Intensive Care unit at Great Ormond St Hospital (GOS). It was decided they were only people who could get to the bottom of why Lennon could not be parted from a ventilator. It took 5 weeks for that day to arrive. I’ll never forget the transport team turning up, and not quiet believing that the day had finally arrived.

Lennon looked so big inside the transport incubator.
As soon as Lennon had arrived at GOS they began their extensive tests. It didn’t take long for them to diagnose Lennon with Chronic Renal failure – he had 1 cystic kidney and a small ball of cysts where the other should have sat. They also diagnosed him with pan hypopituitarism – his little body was not producing thyroxine, or growth hormone and they suspected that his adrenal glands were also dysfunctional. The most significant finding was in Lennon’s heart – His PDA (the shunt that snaps closed when a baby is born) was gapping open. The cardiac surgeon had said it was one of the biggest he had ever seen.
Once Lennon had undergone cardiac surgery he was taken off the ventilator. And after a 2 week stay at GOS Lennon was discharged back to Lister and into a cot for the first time! I couldn’t have been happier – my little soldier had cheated death yet again and maybe this time we were coming to the end of our Special care journey.

We prepared for Lennon to come home with us.
For us to finally be his Mummy and Daddy.
For us to be able look after him and make all the decisions.
We had resuscitation training and our house was fitted with home oxygen. We collected a prescription of special milk and a ton of medication. We borrowed saturation and apnea monitors, blood pressure and suction machines from the hospital. Our small flat was over taken with medical supplies. I was scared, but above all so very excited to bring our son home for the first time. At various points over the 6 months I doubted this day would ever come. I always thought Lennon was not destined to come home, go to school, or grow up. I could never picture at home – no matter how hard I tried.

We were allowed to take Lennon off the ward for small amounts of time to get used to looking after him without the support of the amazing nurses that we had come to rely on over the last 6 months. We spent a night in a bedroom on the ward the night before we brought Lennon home.
Neither of us slept.
I spent the whole night either holding Lennon or staring at him. Disbelieving the day had finally arrived.
On 24th May 2007, after 6 months, we walked out of the Special Baby Care unit. I carried Lennon in his car seat, with an oxygen cylinder on my back. Down the very corridor I had spent the last few months walking up down, watching mothers leaving the delivery suite holding their babies. Those mothers haunted me – all I wanted was to walk out of the hospital holding my baby. Finally it was my turn.

Our Special Care community nurse followed us home. She stayed with us until we had settled in and felt confident enough for her to leave.
I was ecstatic!
Poor Lennon was moved about like a doll. I placed him in his Moses basket, into the swing we had brought him months earlier. I cuddled him, stared at him – Almost trying to make up for the last 6 months. I still could not believe that my precious baby boy had survived and was finally well enough to come home with us.
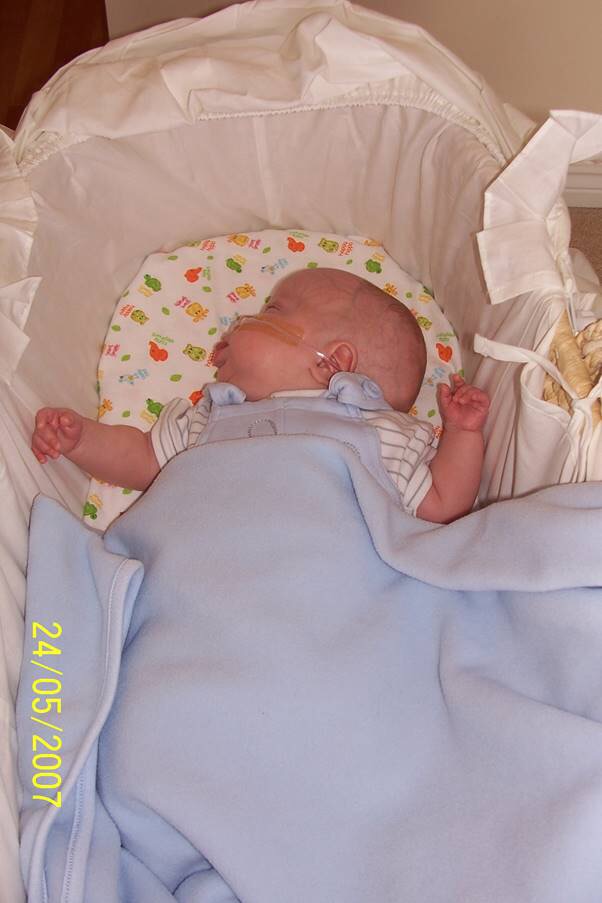
That night before we went to bed, I gave Lennon his medications before his last feed of the day.
He went blue and floppy in my arms.
I called for Ian, Lennon had stopped breathing.
He still had a pulse.
I laid him onto our bedroom floor and started CPR whilst Ian rang an ambulance.
My adrenaline kicked in and I knew what I had to do – I didn’t even have to think about it. By the time the ambulance had arrived Lennon was breathing again. I had saved his life. Thank goodness for the CPR training I had done before leaving hospital.
I felt numb.
Lennon ended up back in hospital that night, and a new journey began. 6 months in Special Care for not even 24 hours at home.
So much happened over those 6 months, and I learnt so much. I learnt that things aren’t always as they seem. I learnt the meaning behind the saying ‘The best laid plans of mice and men often go awry’ – no matter how much we or anyone else planned, the potential for something to go against that plan was always there. Lennon often wrote his own rule book!
The biggest lesson I learnt from being in NICU was patience – I never had any before Lennon was born. I struggled to wait for anything.
Patience was the main ingredient I needed to help me get through the 10 years that followed.

Previous blog post – What does Nascot Lawn mean to me?

